New Patients
(732) 813-3564
Existing Patients
(732) 639-3495
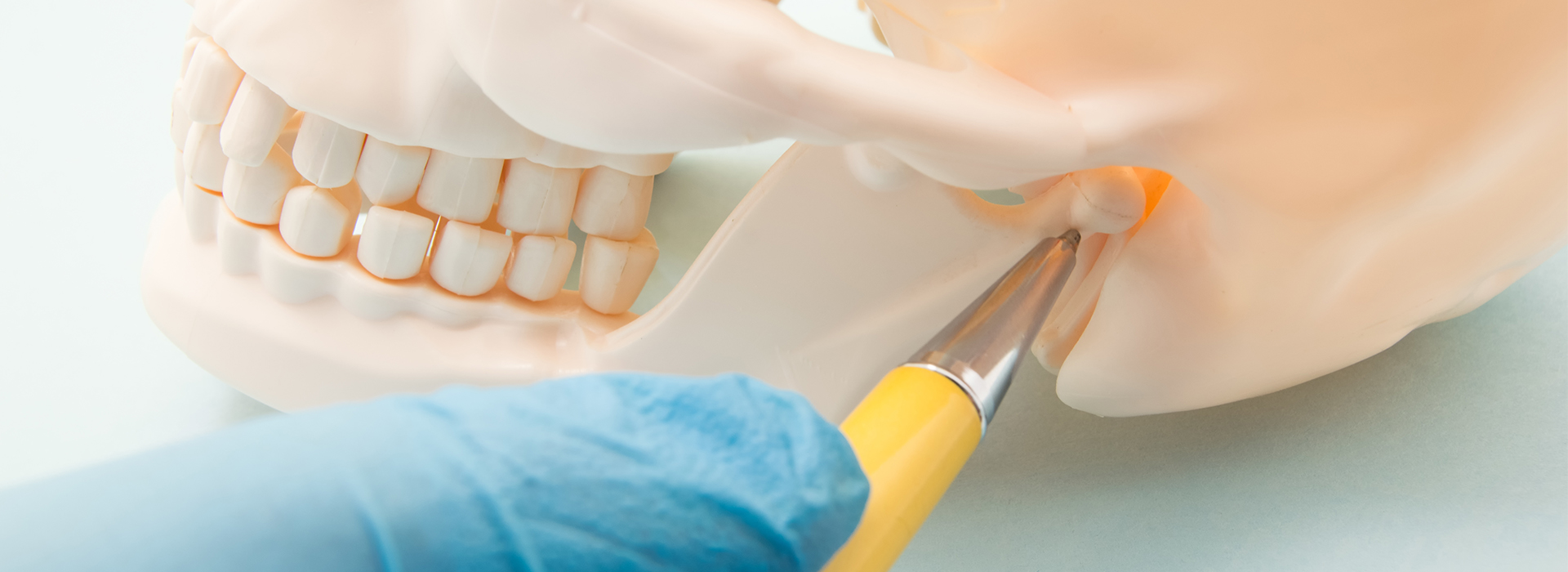
The temporomandibular joint (TMJ) is the small but remarkably complex hinge that connects your lower jaw to the skull. Unlike a simple hinge, each TMJ combines rotational and gliding motions that let the jaw open, close, and move side-to-side. Those combined actions make everyday tasks like speaking, chewing, and yawning possible, but they also introduce more opportunities for stress and wear than many other joints in the body.
Two TMJs — one on each side of the face — must function in near-perfect coordination. When one side is tight, misaligned, or inflamed, the other side and the muscles that control jaw movement often compensate, creating a chain reaction of discomfort. That interdependence is why issues in this area frequently present with symptoms that extend beyond the jaw itself.
Understanding how the TMJ works helps patients appreciate why even subtle changes in bite, muscle tension, or joint health can produce a wide variety of symptoms. For clinicians, it underscores the importance of a comprehensive approach that considers teeth, muscles, ligaments, and nervous system input together rather than in isolation.
TMJ disorders rarely have a single cause; instead, they arise from a combination of mechanical, medical, and lifestyle factors. Teeth grinding (bruxism) and clenching are common culprits because they place repetitive, high-pressure loads on the joint and surrounding muscles. Acute trauma to the jaw, such as a fall or sports injury, can also damage joint structures or shift the position of the disc that cushions the condyle.
Systemic conditions like osteoarthritis or rheumatoid arthritis can affect the joint’s cartilage and bone, leading to degenerative changes that produce pain and limited motion. Hormonal influences and genetic predispositions play a role for some patients, which helps explain why TMJ problems are more frequent in certain populations.
Behavioral contributors such as poor posture, chronic stress, and repetitive chewing habits (for example, prolonged gum chewing) exacerbate strain on the TMJ complex. Because multiple factors often overlap, successful management usually starts by identifying the dominant contributors for each patient rather than applying a one-size-fits-all remedy.
TMJ disorders can present with a varied symptom profile that extends far beyond localized jaw pain. Many patients notice ear-related complaints — earaches, a feeling of fullness, or intermittent ringing (tinnitus) — even when their hearing is normal. Headaches that originate near the temples or at the base of the skull are also common and can be misattributed to sinus or tension headache conditions.
Other frequent signs include clicking, popping, or grinding noises when opening or closing the mouth, episodes of the jaw catching or locking, and difficulty achieving a comfortable bite. Muscle fatigue in the face and neck, unexplained tooth sensitivity, and even changes in facial muscle appearance can accompany more advanced dysfunction. Importantly, symptoms may fluctuate over time and can be provoked by stress or specific jaw activities.
Because these complaints overlap with other medical and ENT conditions, patients should receive a careful evaluation. Persistent or worsening symptoms merit professional assessment rather than prolonged self-diagnosis, especially when daily activities like eating or speaking are affected.
An effective diagnostic process begins with a detailed history and a focused physical exam. The clinician will ask about symptom timing, triggers, prior injuries, sleep habits, and any history of tooth grinding. During the exam, jaw movement range, joint sounds, muscle tenderness, and bite alignment are carefully assessed. Observing how the teeth meet and how the facial muscles behave during function provides important clues.
When indicated, imaging supplements the clinical exam. Panoramic films, cone-beam CT scans, and, in select cases, MRI can reveal joint structure, disc position, degenerative changes, or signs of trauma. These tools help differentiate TMJ-related problems from dental pain, sinus issues, or neurologic sources and guide a targeted treatment plan.
Because TMJ conditions often sit at the intersection of dental and medical specialties, coordination of care can improve outcomes. Your dentist may collaborate with physical therapists, ENT physicians, or rheumatologists when systemic disease or complex musculoskeletal dysfunction is suspected.
Treatment for TMJ disorders typically starts with conservative, reversible measures focused on reducing pain and normalizing function. Oral appliances such as stabilization splints or night guards help reduce excessive forces from clenching and grinding, protect teeth, and allow irritated muscles and joint tissues to recover. Bite interventions aimed at permanently changing dental occlusion are used selectively and only after careful evaluation.
Noninvasive therapies — including guided jaw exercises, manual therapy by trained clinicians, posture correction, and stress-management techniques — play a central role in many treatment plans. These approaches target muscular contributors, improve coordination, and teach patients how to modify behaviors that perpetuate symptoms. Short-term use of analgesics or anti-inflammatory medication may be recommended by a clinician to control acute pain while other therapies take effect.
For persistent cases that do not respond to conservative care, minimally invasive procedures such as intra-articular injections or arthrocentesis may be considered. Surgical options are reserved for well-defined structural problems and are approached cautiously with multidisciplinary input. Throughout every step, clear communication and realistic expectations help patients make informed decisions about their care.
Successful management of TMJ disorders hinges on partnership between patient and clinician. Early evaluation and a staged approach to care — beginning with low-risk interventions and advancing only as necessary — tend to produce the best combination of symptom relief and function restoration. Regular follow-up lets the dental team track progress and tailor therapies as needs evolve.
When you seek care, bring a concise history of symptoms, any prior treatments, and details about habits such as nighttime clenching or daytime jaw tension. This information helps your clinician prioritize diagnostic steps and recommend practical strategies you can start right away. If lifestyle or medical factors contribute to your condition, coordinated care with other specialists can improve outcomes.
Elegant Dental Arts takes a patient-centered approach to TMJ management, combining thorough evaluation with evidence-based therapies designed to reduce pain and restore function. If you live in or near Freehold, NJ, and are experiencing jaw discomfort or related symptoms, our team can help you understand the likely causes and map a sensible course forward.
In summary, TMJ disorders are multifaceted conditions that require careful assessment and individualized care. If you have persistent jaw pain, joint noises, limited movement, or related headaches and ear symptoms, contact us to learn more about evaluation and treatment options. Our team is available to answer questions and help you take the next step toward greater comfort and function.
Temporomandibular joint (TMJ) disorders are a group of conditions that affect the joints and muscles responsible for jaw movement. They can involve the joint surfaces, the cushioning disc, the surrounding ligaments, and the muscles that control chewing and facial expression. Because the TMJs combine hinge and sliding motions on both sides of the face, even small changes can disrupt normal function and cause pain or restricted movement.
TMJ disorders range from transient muscle strain to longer‑term degenerative or inflammatory problems, and symptoms often fluctuate over time. Diagnosis and treatment focus on identifying the dominant contributors for each patient so care can be individualized. A staged, conservative approach is typically recommended to restore comfort and preserve joint health whenever possible.
TMJ disorders usually result from a combination of mechanical, biological, and behavioral factors rather than a single cause. Common contributors include teeth grinding or clenching (bruxism), acute trauma to the jaw, degenerative joint disease such as osteoarthritis, and systemic inflammatory conditions like rheumatoid arthritis. Habitual behaviors such as poor posture, prolonged gum chewing, and chronic stress can further increase muscle tension and joint load.
Genetic predisposition and hormonal influences may make some patients more susceptible, and changes in dental occlusion or tooth wear can alter how forces are distributed across the joints. Because multiple factors often overlap, a careful history and examination are essential to identify which elements are driving a patient’s symptoms. Addressing the primary drivers usually improves outcomes more effectively than isolated symptom treatment.
Symptoms commonly associated with TMJ disorders include jaw pain or tenderness, difficulty opening or closing the mouth, and noises such as clicking, popping, or grinding during movement. Many patients also experience headaches (often near the temples), ear sensations such as fullness or ringing, neck pain, and facial muscle fatigue. These complaints may be intermittent and can worsen with chewing, talking, or periods of increased stress.
Because TMJ problems overlap with dental, neurologic, and ENT conditions, isolated symptoms like ear pain or chronic headache should prompt a comprehensive evaluation if they persist. Episodes of jaw locking, significant changes in bite, or pain that interferes with eating or speaking warrant prompt assessment by a dental professional. Early recognition and targeted intervention can help prevent progression and reduce the need for invasive therapies.
Evaluation begins with a detailed medical and dental history and a focused physical examination of jaw movement, joint sounds, muscle tenderness, and bite relationships. The clinician will ask about symptom timing, sleep habits, grinding or clenching behaviors, prior injuries, and factors that worsen or relieve symptoms. Observing functional movements and palpating muscles and joints provides important diagnostic clues that guide further testing.
When indicated, imaging such as panoramic radiographs, cone‑beam CT (CBCT), or magnetic resonance imaging (MRI) can clarify joint structure, disc position, and degenerative change. Because TMJ disorders often involve overlapping dental and medical issues, dentists commonly coordinate care with physical therapists, ENT specialists, or rheumatologists for comprehensive management. This multidisciplinary approach helps ensure accurate diagnosis and an appropriate treatment plan.
Initial treatment typically emphasizes conservative, reversible therapies aimed at reducing pain and normalizing jaw function. Common measures include custom oral appliances such as stabilization splints or night guards to reduce excessive forces from clenching, guided jaw exercises to improve mobility and coordination, manual therapy from trained clinicians, and behavioral strategies to manage stress and modify harmful habits. Short‑term use of analgesics or anti‑inflammatory medications may be recommended to control acute symptoms while other therapies take effect.
Posture correction and ergonomic adjustments can also reduce strain on the jaw and neck, and patients often benefit from education about jaw rest positions and activity modification. These noninvasive strategies form the foundation of most treatment plans and are usually effective for many patients when applied consistently. Progress is monitored with regular follow‑up so therapies can be adjusted as needed.
Oral appliances such as stabilization splints and night guards are designed to redistribute biting forces, protect teeth from wear, and reduce excessive loading of the jaw muscles and joints. They work by creating a stable occlusal surface that encourages more relaxed muscle activity and can interrupt damaging grinding or clenching patterns during sleep. A well‑fitted appliance also gives irritated muscles and joint tissues time to recover, which often reduces pain and improves function.
Appliance therapy is a reversible and conservative intervention that should be custom fabricated and periodically re‑evaluated by a dental professional. While many patients experience meaningful symptom relief, appliances are part of a broader plan that may include exercises, behavioral changes, and other therapies. Long‑term occlusal adjustments or irreversible dental procedures are considered only after careful evaluation and when clearly indicated.
Physical therapy and manual therapy are recommended when muscular dysfunction, restricted range of motion, postural imbalance, or coordination problems are significant contributors to a patient’s TMJ symptoms. Trained therapists use hands‑on techniques, soft tissue mobilization, joint mobilization, and supervised exercise programs to restore mobility, decrease muscle tension, and improve neuromuscular control. These interventions often complement dental appliance therapy and help patients relearn healthy movement patterns.
Home exercise programs, posture training, and ergonomic advice are commonly taught so patients can continue progress between clinic visits. In many cases, combining physical therapy with dental care and behavioral strategies produces better and more durable outcomes than either approach alone. Coordination between the dentist and therapist helps ensure that interventions are synergistic and aligned with the overall treatment goals.
Surgical intervention is reserved for a small subset of patients with clearly defined structural problems that do not respond to comprehensive conservative and minimally invasive care. Indications may include severe internal derangement with persistent functional impairment, advanced joint degeneration, or specific traumatic injuries that have failed to improve with other treatments. Options range from arthrocentesis and arthroscopy to open joint procedures and, in rare cases, joint reconstruction or replacement.
Because surgery carries higher risks and variable outcomes, it is approached cautiously and typically involves collaboration with oral and maxillofacial surgeons, rheumatologists, and other specialists as appropriate. A thorough informed consent process and realistic discussion of expected benefits, limitations, and recovery are essential. Whenever possible, conservative and reversible therapies are exhausted before considering operative solutions.
Yes, TMJ disorders commonly produce headaches and ear‑related symptoms because the TMJs and surrounding muscles share nerve pathways with areas around the temples and ears. Patients may report temple or tension‑type headaches, ear fullness, intermittent ringing (tinnitus), or a sensation of ear pain even when hearing is normal. Muscle referral patterns and altered joint mechanics can create symptoms that mimic primary headache or ENT conditions, which is why careful evaluation is important.
When ear or head symptoms are present, clinicians assess both dental and medical causes and may collaborate with ENT physicians or neurologists if needed. Treating the underlying jaw dysfunction—through appliances, therapy, and habit modification—often reduces referred head and ear symptoms. Persistent or atypical neurologic or auditory signs should prompt expedited medical referral to rule out non‑dental causes.
Successful long‑term management of TMJ disorders depends on an ongoing partnership between you and your dental team, focused on early evaluation, staged treatment, and regular follow‑up. Bring a clear history of symptoms, triggers, and any prior treatments to appointments so the clinician can prioritize diagnostic steps and tailor a plan that targets your specific contributors. Consistent adherence to home exercises, appliance use, and behavior changes such as stress management and posture correction plays a major role in achieving durable improvement.
At Elegant Dental Arts in Freehold, NJ, the care team emphasizes individualized assessment and evidence‑based therapies while coordinating with allied specialists when systemic or complex musculoskeletal issues are suspected. Regular monitoring allows your clinician to adjust therapies as your condition evolves and to advance interventions only when necessary. Open communication, realistic expectations, and a focus on conservative care typically produce the best balance of symptom relief and functional restoration.

