New Patients
(732) 813-3564
Existing Patients
(732) 639-3495

Most dental care focuses on preserving natural teeth, but there are times when removal is the most responsible option. An extraction can stop the spread of infection, prevent damage to neighboring teeth, and resolve sources of persistent pain. Deciding to extract a tooth is a clinical judgment made after careful evaluation of the risks and benefits for your long-term oral health.
Common clinical scenarios that lead to extraction include teeth that are too damaged to restore, severely infected teeth that threaten nearby structures, problematic third molars, and teeth that interfere with orthodontic treatment. Pediatric cases can also require removal when a primary tooth is over-retained and preventing a permanent tooth from erupting properly. Each situation is unique, and treatment plans are tailored to the individual’s overall health and dental goals.
When extraction is recommended, your care team will prioritize preserving function and appearance wherever possible. That may include planning for future restoration, employing techniques to preserve bone, or coordinating care with specialists when a surgical approach is required. The aim is always to protect your oral health while minimizing discomfort and disruption.
We approach every extraction as part of a larger treatment strategy rather than an isolated event. Early communication about expectations, treatment sequencing, and replacement options helps patients feel informed and confident about the next steps in their care.
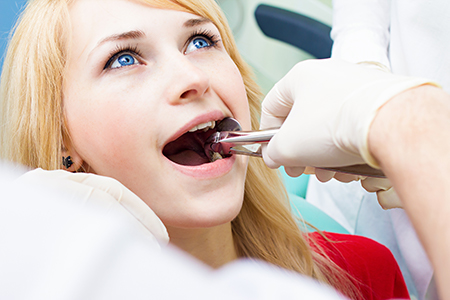
Before any extraction, we review your medical and dental histories to identify factors that influence safety and healing. That includes current medications, chronic health conditions, prior reactions to anesthesia, and any recent illnesses. This information guides decisions about blood-thinning medications, antibiotic needs, and whether medical clearance is recommended.
Imaging is a key part of the assessment. Digital radiographs provide a clear picture of root shape, adjacent anatomy, and bone levels, allowing us to plan a precise and predictable procedure. In cases where additional detail is necessary, three-dimensional imaging may be used to clarify complex root positions or the proximity to nerves and sinuses.
We also discuss anesthesia and comfort measures up front. Most extractions can be performed with local anesthesia, but we offer additional options — including nitrous oxide and oral sedation — for patients who need greater relaxation. Whatever the approach, the team will explain expectations, pre-procedure instructions, and any medication adjustments so you arrive prepared and informed.
Extractions fall into two broad categories: straightforward removals when a tooth is fully visible and uncomplicated, and surgical extractions when access is limited or the tooth’s structure is compromised. Regardless of the category, the priority is a controlled, atraumatic technique that protects surrounding tissues and promotes predictable healing.
For many teeth that are erupted and stable, a simple extraction is performed. The area is anesthetized thoroughly, the supporting tissues are gently loosened, and forceps are used to remove the tooth. This approach is efficient and allows for an uncomplicated recovery in most cases. If you have anxiety about the procedure, we can discuss appropriate sedation options beforehand to make the experience more comfortable.
A simple extraction focuses on minimal disruption to the socket and surrounding bone. After numbing, the tooth is mobilized and removed with controlled traction. We take steps to shape the socket as needed and provide instructions to support clot formation and initial healing. Sutures are rarely required for straightforward cases but may be used when helpful for comfort or tissue management.
Surgical extractions are used for teeth that are fractured at the gumline, ankylosed, impacted, or when roots are curved or unusually positioned. This technique may involve a small incision, removal of a bit of bone, and sectioning the tooth for safe removal. In some complex cases we collaborate with or refer to an oral and maxillofacial surgeon to ensure the most appropriate surgical expertise is applied.
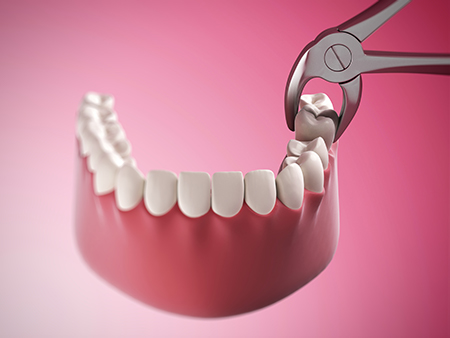
How you care for the extraction site in the first 24–72 hours has a major impact on comfort and healing. Applying firm, steady pressure with gauze helps the body form the initial clot that seals the socket. If bleeding persists beyond the expected period, contacting the office promptly allows us to provide targeted guidance.
Protecting the clot is essential. Avoid actions that may dislodge it — such as rinsing vigorously, using a straw, or smoking — during the critical early phase of healing. Follow prescribed medication directions for antibiotics and pain relief, and take any recommended anti-inflammatory medication to reduce swelling and discomfort.
Cold application and dietary adjustments can make a big difference in early recovery. Intermittent ice reduces swelling during the first day, and choosing soft, lukewarm foods minimizes irritation. Maintain gentle oral hygiene routines, taking care to avoid direct scrubbing of the extraction site; a mild saltwater rinse can be introduced once advised to help keep the area clean.
We schedule follow-up visits when sutures are present, the extraction was complex, or when additional monitoring is needed. If you notice signs such as persistent and worsening pain, increasing swelling after the first 48 hours, fever, or a foul taste that does not resolve, contact the office so we can evaluate and intervene if needed.
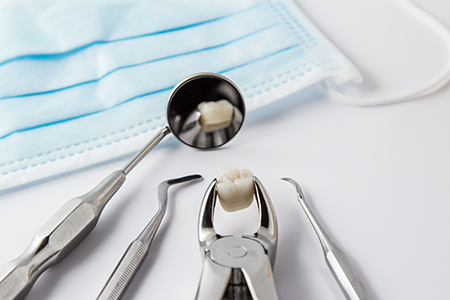
Removing a tooth is often the first step in a longer restorative plan. Preserving jawbone and preparing the site for future replacement are important considerations. When appropriate, techniques such as socket preservation or bone grafting can be used at the time of extraction to maintain ridge contours and support future implant placement.
Replacement options are chosen based on the patient’s overall oral health, aesthetic goals, and functional needs. Fixed solutions such as dental implants and bridges can restore chewing efficiency and appearance, while removable options remain effective for certain situations. Timing is individualized — some cases are suitable for delayed restoration after healing, while others may benefit from a staged approach.
Coordination of care is key. Whether restorations are completed in our office or in partnership with specialists, treatment sequencing is planned to achieve a stable, healthy outcome. At Elegant Dental Arts, we discuss the pros and cons of each replacement option and tailor recommendations to fit your long-term dental health and lifestyle.
Extractions are a common, well-understood part of dental care when preservation is not feasible or when removal better protects overall oral health. With careful evaluation, clear communication, and thoughtful planning for comfort and restoration, the process can be predictable and well tolerated. Our approach emphasizes safety, minimally invasive technique, and preparation for the best possible long-term result.
If you have questions about whether an extraction is recommended for you or would like to discuss replacement options and recovery in detail, please contact us for more information.
The most common reasons for tooth loss include advanced periodontal disease, extensive tooth decay, and facial trauma. According to statistics, gum disease is responsible for close to 70% of tooth loss in adults. Although less frequent than the preceding three reasons, it should also be noted that specific diseases, drugs, smoking, and poor nutrition contribute to the risk of tooth loss.
The Centers for Disease Control and Prevention report that in the United States, an average of 12 teeth (including the wisdom teeth) are lost by the age of 50. Also, 26% of adults between 65 and 74 years of age have lost all their teeth.
Every patient and every situation is different. However, when a tooth and the surrounding tissues are numbed with a local anesthetic, you should only expect to feel a bit of pressure, but no pain as the tooth is being loosened from the surrounding tissues and extracted. For patients who are apprehensive and for some surgical extractions, our office will discuss our options in dental sedation to provide further relaxation and reduce any sense of discomfort.
While it's normal to feel some tenderness and swelling following an extraction, the degree of these sensations can vary. It mostly depends on the complexity of the extraction and the body's response to the procedure. We'll recommend or prescribe the appropriate pain medication to help ensure your comfort and give you specific instructions for maximum effectiveness and safety.
Typically, the recovery period following a simple extraction is shorter than a surgical extraction. However, a patient's overall health, habits, the size and location of the tooth, and other variables can influence recovery and healing. To speed up the recovery and avoid any complications, patients must follow the given at-home instructions diligently. We'll carefully review what to expect following your procedure and go over your post-op instructions.
Smoking interferes with blood clot formation, which is an essential first step in the healing process. Blood clot formation not only provides a protective layer to cover the underlying exposed bone and nerve endings, but it also supports the growth of new tissue. Cigarette smoke also contains chemical toxins that can disrupt the healing process and lead to problems such as continued inflammation, infection, or dry socket.
In a very small percentage of cases, a condition known as dry socket can develop in the aftermath of a dental extraction. This painful condition can arise when the blood clot in the extraction site doesn't form properly or gets dislodged. With dry socket, you may experience throbbing pain and symptoms such as bad breath and an unpleasant taste in your mouth. As skilled providers of care, our office will provide immediate treatment to alleviate your discomfort and promote healing.
The last teeth in your mouth to develop, wisdom teeth often do not have enough room to fully erupt or may be positioned in the wrong direction. These issues can affect your dental health as well as overall wellbeing. While some individuals never develop all their wisdom teeth, and a few have sufficient space for them, there are many people with partially or fully impacted third molars. Our office will monitor the development, position, and health of your wisdom teeth and will advise you if and when extractions are indicated.
After a tooth is removed, bone-grafting material is sometimes placed in the socket to promote healing and encourage new bone development. This procedure is often performed to support the eventual and successful placement of a dental implant.
At the office of Elegant Dental Arts, we strive to make dental care affordable and accessible. Depending on the type or complexity of the extraction and other variables, the cost of the procedure can vary. Based on our diagnostic findings, our office will inform you of the healthiest choices in care, explain the fees, discuss insurance coverage, and explain your payment options.
Many dental plans offer some level of coverage for tooth extractions. We'll advise you if your plan covers the full cost of the procedure and if there is any out-of-pocket expense. Our business office will work with you to maximize your insurance benefits as much as possible while helping you minimize any out-of-pocket expenses.
An extraction is recommended when a tooth cannot be restored to a healthy, functional state or when it endangers adjacent teeth and tissues. Common indications include severe decay that reaches the tooth root, an infection that does not respond to conservative treatment, a fractured tooth that cannot be rebuilt, and certain cases of advanced periodontal disease. The decision to remove a tooth follows a careful clinical evaluation that balances immediate needs with long-term oral health goals.
In some situations, extractions are performed to address developmental or mechanical problems, such as impacted third molars that threaten nearby structures or primary teeth that block proper eruption of permanent teeth. Orthodontic treatment can also create scenarios where removal is the best option to achieve proper alignment and bite function. Your provider will review alternatives and explain why extraction is the most responsible course when preservation is not feasible.
Simple extractions are used for teeth that are fully erupted and easily accessible; they are typically done by gently loosening the tooth and removing it with forceps after local anesthesia. This approach focuses on minimizing trauma to the socket and surrounding bone to support predictable healing and a straightforward recovery. Simple extractions seldom require sutures and are often completed quickly in a single visit.
Surgical extractions are indicated when access is limited or the tooth is compromised by fracture, unusual root anatomy, ankylosis, or impaction. These procedures may involve a small incision in the gum, removal of a small amount of bone, and sectioning the tooth for safe removal; they are planned carefully to protect adjacent nerves and sinuses. In complex cases, collaboration with or referral to an oral and maxillofacial surgeon ensures specialized surgical expertise and the best possible outcome.
Preparation begins with a thorough review of your medical and dental history, including current medications, chronic health conditions, allergies, and previous reactions to anesthesia. This information helps determine whether medication adjustments, such as temporary changes to blood thinners, or medical clearance from your physician are necessary before the procedure. Diagnostic imaging, including digital X-rays or three-dimensional scans when needed, gives a clear view of root shape and nearby anatomy so the team can plan a safe, efficient extraction.
Before the appointment, you will receive instructions about fasting only if sedation is planned and about taking or pausing certain medications as directed by the clinical team. Arranging a ride home is advised for anyone receiving sedation or heavy anxiolytics, and you should plan for a period of rest after the procedure. Clear preoperative communication reduces anxiety and contributes to a smoother experience and recovery.
Most extractions can be performed comfortably with local anesthesia, which numbs the area around the tooth while keeping you awake and responsive. For patients with heightened anxiety or for more complex procedures, supplemental options such as nitrous oxide (laughing gas) or oral sedation can provide additional relaxation while maintaining safety and quick recovery. Deeper levels of sedation are available in coordination with specialists when medically indicated or when extensive surgical intervention is planned.
Your clinician will review the risks and benefits of each option and tailor the approach to your medical history, level of anxiety, and the complexity of the extraction. Pre-procedure instructions will outline fasting requirements and medication guidance for your selected sedation method. Choosing the right comfort strategy helps ensure a controlled, low-stress experience during the procedure.
The first 24 to 72 hours are the most important for clot formation and initial healing, so following post-operative directions helps reduce complications and discomfort. You will be advised to apply firm pressure with gauze to control bleeding, avoid vigorous rinsing, refrain from using straws or smoking, and maintain a soft-food diet while the site stabilizes. Intermittent cold application and over-the-counter or prescribed analgesics can help manage swelling and pain during the early recovery period.
Maintain gentle oral hygiene away from the extraction site and introduce a mild saltwater rinse only when advised to support cleanliness without disturbing the clot. Most patients experience gradual improvement in pain and swelling over several days, and routine follow-up is scheduled when sutures are used or the extraction was complex. If symptoms such as increasing pain after 48 hours, persistent bleeding, fever, or unusual drainage occur, contact the office promptly for evaluation.
Dry socket, or alveolar osteitis, is a complication in which the blood clot that normally protects the extraction site is dislodged or fails to form, exposing underlying bone and nerves and causing increased pain. It most commonly appears two to four days after extraction and can be accompanied by a foul taste or odor and radiating pain. Certain risk factors, such as tobacco use, poor oral hygiene, traumatic extractions, and prior history of dry socket, increase the likelihood of this condition.
Prevention centers on protecting the formation and stability of the clot: following post-operative instructions, avoiding smoking and suction-like actions, adhering to dietary and activity guidelines, and maintaining cleanliness without vigorous rinsing. When risk is elevated, clinicians may take extra steps such as atraumatic surgical technique, placing protective dressings, or providing targeted postoperative instructions to minimize the chance of dry socket. Early recognition and treatment can control pain and promote healing if the condition develops.
Antibiotics are not routinely required for every extraction and are prescribed based on specific clinical factors rather than as a standard precaution. Indications for antibiotic use include active spreading infection, compromised immune status, certain medical conditions that increase infection risk, or when extraction involves extensive surgical manipulation that raises concern for postoperative infection. Your clinician will weigh the benefits and risks of antibiotics in the context of your overall health and the nature of the procedure.
When antibiotics are indicated, the prescription will be accompanied by clear instructions on dosage and duration and by guidance on monitoring for side effects. It is important to complete the prescribed course as directed and to report any adverse reactions or persistent signs of infection, such as fever or worsening swelling. Judicious use of antibiotics helps protect overall health while reducing unnecessary exposure to medications.
When removal of a tooth is part of a longer restorative plan, techniques such as socket preservation and bone grafting can be employed at the time of extraction to maintain ridge contours and support future implants or prosthetic solutions. Socket preservation typically involves placing graft material and a protective membrane into the extraction site to reduce bone resorption and preserve the height and width of the jaw. These measures help maintain favorable anatomy for later implant placement, bridgework, or other restorations.
The decision to graft and the timing of definitive replacement are individualized based on the condition of the surrounding bone, the presence of infection, aesthetic concerns, and the patient’s overall treatment goals. In some cases, immediate implant placement is appropriate; in others, staged healing followed by restoration is preferred. Your clinician will discuss the pros and cons of each approach and coordinate care to achieve a stable, functional result for the long term.
Extractions are sometimes recommended to create space, correct severe crowding, or improve bite relationships as part of an orthodontic treatment plan. Removing select teeth can facilitate proper alignment, minimize the need for excessive expansion, and help achieve stable occlusion when non-extraction approaches cannot deliver the desired functional or aesthetic outcome. The decision is made collaboratively between the orthodontist and restorative team and is based on thorough diagnostic records and treatment goals.
For younger patients, timing is important to coordinate tooth removal with growth and eruption patterns to guide efficient tooth movement. Conservative alternatives are considered first, and when extraction is chosen, planning includes discussion of future restorative needs and how the extractions will affect facial balance and oral function. Communication about expectations and sequencing helps patients and families understand the role extractions play in comprehensive orthodontic care.
Complex extractions may require multidisciplinary coordination with oral surgeons, periodontists, or restorative specialists to ensure optimal surgical technique and appropriate restorative sequencing. The team reviews diagnostic imaging and medical history, discusses potential referral when advanced surgical skills are needed, and plans for socket preservation or staged restoration as indicated. Clear communication about treatment phases and timelines helps patients understand what to expect and supports continuity of care.
At Elegant Dental Arts we prioritize collaborative planning and patient education so that surgical steps, pain management, and restorative options are aligned with long-term goals. Follow-up visits are scheduled when sutures are placed, when complications are possible, or when additional monitoring is required, and the care team provides clear post-operative instructions and contact information for concerns. This coordinated approach aims to protect oral health, restore function, and support predictable outcomes following extraction.

